Our dental health has moved to a new page to better serve our readers. Please direct your browser to the URL below for our updated blog address to stay up to date on new articles and information. Smiles!
http://www.bellevuefamilydentistry.com/dental-health-blog/

Welcome to our oral health and dental care blog! From Dr. Peter Chien, your gentle family Bellevue Dentist in WA state. We serve the areas of Bellevue, Redmond, Newcastle, Issaquah, Sammamish, and Seattle. Our friendly team is here to assist you in every way we can. Check back often as we frequently post interesting oral health and dental news. www.BellevueFamilyDentistry.com
Wednesday, August 3, 2016
Friday, July 1, 2016
how to get rid of bad dog breath
 |
| Yorkshire showing his teeth :) |
Did you know plaque and tartar buildup is not only bad for us (people) but also bad for our pets, especially dogs! Puppy breath is nice until it develops into "doggie breath" which at that point becomes an annoyance for us. Just as we take care of our kids and our own oral health with toothbrushes and toothpaste, our pet's oral health is important too.
Most pet owners are probably not as attentive to their dogs oral health and hygiene, but our pet dog's teeth and gums need care, just like people's teeth. Recently increases in pet care products (including canine toothbrushes and toothpastes), which help makes taking care of our dog's oral health more readily accessible.
Young pups have 28 primary (baby) teeth; adult dogs have 42 permanent teeth. Majority of dogs exhibit signs and symptoms of gum disease by 3 years of age (or roughly 21 dog years) when all of their adult teeth have come in. Below are some signs of gums disease in dogs to watch for as our dogs mature in age:
GUM DISEASE SIGNS AND SYMPTOMS IN DOGS
- Tartar buildup (looks like a dark yellow or dark black hard residue on the dog's teeth)
- Red, puffy, and bleeding gums
- Bad breath
- Crowded teeth and malocclusion
- Not wanting to eat and weight loss
- Red discharge
- Atypical behavioral change
When one first starts brushing their dog's teeth, initially have the the dog smell and taste the toothpaste (some toothpastes are actually meat flavored!). Start brushing one side of the dog's teeth, and then brush the other side. Take frequent breaks if necessary. Also try to see if you notice any changes or discolorations in your pet's teeth and gums. Make it a fun bonding event!
Take your canine friend to the veterinarian at least once a year for a preventive exam and a dental cleaning (usually performed under general anesthesia) and be sure to inquire if the vet includes an assessment of your dog's oral health. If you have any questions on your dog's dental health please consult your family veterinarian. Woof!
From your friendly family dentist in Bellevue,
Peter Chien, DMD, MPH
www.bellevuefamilydentistry.com
425-614-1600
Wednesday, June 1, 2016
how much radiation from dental x-rays
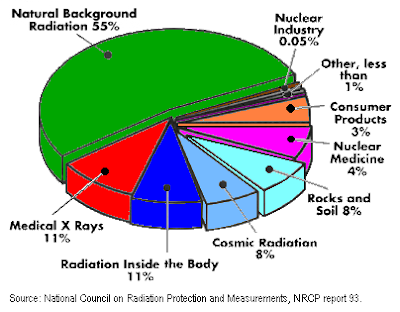 | |
| Background Radiation Sources |
How much radiation am I exposed to with x-rays at the dentist? Are x-rays necessary? An exam with 4 bitewings is about 0.005 mSv, less than one day's worth from natural background radiation, and is the same exposure amount from an airplane flight of ~2 hours. Such are legitimate questions patients may ask when they visit the dentist for their annual checkups and cleanings.
On should consider that EVERYONE is exposed to radiation EVERYDAY. The amount exposed depends on where you live, how much time you spend outdoors, and even your occupation. By far radon is the largest contributor to background radiation. Over 50% of daily radiation exposure comes from radon (radon has no smell, no odor, no taste, no color, and is present in your house due to trapped pressure from the rocks and soil underneath houses and buildings). Other sources of daily radiation include the sun,daily consumables, some tests required at the hospital, external rocks and soils, and various internal elements in the human body. In comparison, dental x-rays amount to less than 0.1% of the annual radiation exposure.
- WHY ARE X-RAYS NECESSARY AT THE DENTAL OFFICE?
- Diagnose cavities between your teeth
- Check for cavities underneath crowns and fillings
- Check for bone loss and periodontal disease
- Make sure your hard tissue and soft tissue adjacent to the oral and maxillofacial structures are normal
- Check the position of your wisdom teeth and evaluate for possible tooth extraction
- Examine how your children's baby teeth are erupting
- Orthodontically evaluate the positioning of your teeth and determine if braces and/or invisalign are options to correct any occlusal misalignment
- Check for missing permanent teeth
- Evaluate pathology, swelling, cancer, and many others...
From your gentle dentist in Bellevue and Redmond,
Peter Chien, DMD, MPH
www.bellevuefamilydentistry.com
(425) 614-1600
Labels:
dental x-rays,
necessary,
radiation
Location:
Bellevue, WA, USA
Monday, May 2, 2016
root canal retreat or extraction
 | |
| Failed root canal treatment |
Consider real life scenario A: Patient "Mary" had a root canal and a crown on a lower right molar a few years ago. The tooth became symptomatic, and upon evaluation and x-ray bacteria had infiltrated the root canal and was reinfected. Mary consulted a well respected endodontist, and the two decided to treat the tooth with a root canal retreatment and apico surgery. The tooth's symptoms resolved; three years later pain and swelling came back where I saw the patient for an evaluation of the tooth. X-ray showed infection (radiolucency) around the retreated root canal tooth. Mary was presented two options at that time: go to an endodontist to have the tooth evaluated for retreatment or extraction and implant, or try antibiotics to resolve the swelling. Mary elected the antibiotic route and was placed on broad spectrum antibiotics; 2 weeks later the pain persisted where Mary was then seen by an endodontist. The endodontist concluded that one of the roots had excessive resorption and probable fracture, and recommended extraction with future implant.
Let's then consider real life scenario B: Patient "Todd" had a root canal and crown on a lower left molar a year ago. Though the tooth presented with no symptoms, a routine x-ray suggested the tooth's root canal was beginning to get infected. Todd was referred to an endodontist, who determined the tooth was beset treated with a root canal retreatment. Upon endodontic retreatment and currently four years later the tooth remains symptom free with a x-rays showing the tooth with crestal bone healing.
So in what situation is it feasible to retreat the failing root canal? Or is it more worthwhile to just extract the tooth and replace it with an implant of bridge? Each situation is clinically different and would likely depend on the extent of the infection, how extensive the symptoms, amount of bone loss surrounding the roots, periodontal disease involvement, and the history of the tooth. If you have a tooth that previously had a root canal and have been experiencing discomfort and/or swelling, be sure to consult your family dentist and endondontist and have the tooth evaluated for restorability.
From the desk of your gentle Bellevue dentist,
Peter Chien, DMD, MPH
www.bellevuefamilydentistry.com
(425) 614-1600
Friday, April 1, 2016
Broken tooth while biting down
 |
| Broken Tooth Fractured Molar |
Have you ever bit down during lunch or while eating and chewing you suddenly noticed you broke off a piece of your tooth? You look at the broken tooth part and wonder what part of the tooth may be. If this accident ever occurs it may be emergency dentistry and your tooth may or may not have pain. You should consult your family dentist as soon as possible to address this incident.
What may have caused your tooth to break?
- The tooth had a cavity and this part of the tooth became weakened and broke off
- Teeth, especially molars and premolars, are subject to chewing and night time and day time grinding stress. Over the years these teeth may have developed small and tiny fractures and cracks. If these fractures get large enough, they may eventually give away and break off.
- The tooth had a large filling and during chewing and biting this filling gave away. Sometimes it is also possible for a portion of the tooth to break off along with the filling.
- The previously had a root canal and was filled with a temporary filling or just had a large restoration. Teeth with a root canal are generally more brittle and without a dental crown the tooth make break.
- The tooth may have a filling that may have failed due to age and use.
- A piece of tooth is already broken and over time, this tooth became weakened due to tooth decay and use.
- Your teeth may have shifted, causing your teeth to be out of normal alignment. And as such the part of the tooth that is "out of position" may be prone to fracture.
Will I have pain due to a broken tooth?
It is possible not to have any feeling or sensation when a piece of the tooth has broken, especially if the tooth already had a root canal; not always the case though, as if a root canal tooth develops an infection, one may have sensitivity.If the part of the tooth broken off is small and contained within the enamel, it is also possible not to have any discomfort. Otherwise, it will be normal to have soreness and cold, hot, and eating sensitivity. If part of the tooth's nerve is exposed this may be very painful and uncomfortable.
What are treatment options to fix the broken tooth?
Your dentist will do a comprehensive evaluation of the tooth and supporting gum and bone structures. Treatment options can range from doing nothing to smoothing part of the tooth, or a small filling if the broken portion is small enough. If the damage is more extensive, a full coverage crown or root canal may be required, or even possible extraction if the damage is not restorable.If you have any questions or concerns regarding a broken tooth, be sure to consult your family dentist for the best possible care and treatment.
From your gentle family dentist,
Dr. Chien
www.bellevuefamilydentistry.com
(425) 614-1600
Labels:
broken teeth,
broken tooth,
Porcelain Crowns
Location:
Bellevue, WA, USA
Tuesday, March 1, 2016
Tooth sensitive to sweets and sugar
 |
| Ouch! My tooth hurts when I eat sweets! |
CAUSES OF TOOTH SWEET SENSITIVITY
- tooth decay due to presence of bacteria and exposed enamel and/or dentin
- exposed dentin and enamel from excessive toothbrushing and tooth grinding (ie. bruxism habit). Dentin and enamel exposure can also result from excessive eating and drinking acidic foods.
- broken tooth, exposing the tooth's inner layer
- lost filling, thereby exposing enamel and dentin
- tooth's nerve is exposed
SIGNS AND SYMPTOMS OF SUGAR SENSITIVITY
When eating foods or ingesting drinks that are sugary and these foods cause your tooth to be sensitive or painful, your tooth may be sweet sensitive. Usually once the food or drink is fully ingested the sensitivity will immediately go away.WHY DOES SUGAR CAUSE MY TOOTH TO BE SENSITIVE?
Sugar can be quite addictive and delicious, but sugars can also cause enamel to be worn away. The sweets in deserts, sugary carbonated drinks, etc. contain high amounts of carbohydrates that interact with bacteria in your mouth to form acids. Such acids cause enamel erosion, and as such higher amounts of sugar leads to greater acid production, and increased chance of sensitivity. Repeated constant exposure of sugars may eventually lead to tooth decay.HOW TO TREAT SWEET SENSITIVE TEETH
If a tooth is sensitive to sweets, have your dentist evaluate the tooth. If it is due to tooth decay, a filling may be needed. If the sensitivity is due to a broken tooth, a filling or full coverage crown and root canal may be required. If the sweet sensitivity is due to exposed enamel or dentin, a toothpaste designed for sensitive teeth may help, such as Sensodyne or Colgate Sensitive or Floridex.A proper diet low in processed foods with high sugar contents like soda, cookies, and candies will help. Instead load up on fresh vegetables, fruits, and water. A diet low in acid may also help.
Brushing your teeth twice and flossing regularly is also recommended.
If you have any questions or concerns why your tooth is sensitive to sweets and sugars, be sure to consult your family dentist and dental hygienist.
Your gentle dentist in Bellevue and Redmond,
Peter Chien, DMD, MPH
www.bellevuefamilydentistry.com
(425) 614-1600
Location:
Bellevue, WA, USA
Monday, February 1, 2016
Dental crown came off
 |
| Recementing a dental crown that fell off |
"My dental crown fell off when I was eating, what do I do?" Though it's rare, dental caps or crowns may occasionally come off the tooth. If the crown does come off, it's important to see your dentist right away, and may be considered an emergency dental visit especially if the tooth is sensitive.
What should I do when my crown comes off?
First recommendation is to have your family dentist evaluate the tooth and the crown to make sure both the tooth underneath the crown attaches to and the crown are in stable condition. If both the tooth and the cap is stable, it may be a matter of just recementing the crown back on. If the tooth or crown is not stable, other treatment may be necessary.Nonetheless it is suggested one sees the dentist as soon as possible to prevent further possible damage to the tooth the crown was attached to. The dentist will perform a limited exam and may take a couple of peri-apical digital x-rays to determine if there is damage or infection to the tooth.
If you are on vacation or a business trip and are not able to have access to dental care, you can purchase temporary dental cement at a pharmacy to temporarily place the crown back on the tooth until you see a dentist. Alternatively you can also try vasoline to create temporary seal between the tooth and the crown. If neither temporary dental cement nor vasoline is obtainable, place the crown in a zip-lock bag and be sure bring the crown in for evaluation.
What caused the crown to come off?
- The cement between the crown and tooth has "worn out."
- There is a cavity or tooth decay underneath the crown, and the tooth has weakened
- Part of the tooth the crown adhered to has weakened from years of use, the tooth has broken off along with the crown.
- There was not quite enough ideal tooth structure remaining when the crown was placed (may have been due to extensive tooth decay or tooth fracture, and the crown was done to try and save the tooth from being extracted).
- The tooth was naturally short or small to begin with, and hence the crown may not have ideal sufficient tooth structure to hold the crown in place over sustained period of time. This is most common with second molars.
- Due to excessive use and chewing, the crown and along with a portion of the tooth underneath was "knocked" out. This may be prevalent in those who grind or clench their teeth.
What are treatment options for the crown that fell off?
If the cement has weakened over time, the dentist may be able to recement the "old" crown back on with new dental cement. This is by far the most conservative and ideal outcome.If there is extensive decay or fractured tooth structure, the decay and weakened tooth portion may need to be removed and re-evaluated. If the decay is small, a recement of the crown is possible. A new crow may also be necessary if there is extensive damage. If the decay or fracture is extensive and the nerve is affected, a root canal and new crown, or even an extraction may be required if there is insufficient tooth structure for a crown to adhere to.
If the crown has fallen off and it has been a few weeks or months since the crown has been off, this increases the chance the tooth may move and be subject to decay and fracture.
If you have any questions or concerns about a crown that has fallen off, please consult your family dentist as soon as possible.
From the desk of your gentle dentist in Bellevue,
Peter Chien, DMD, MPH
(425) 614-1600
www.bellevuefamilydentistry.com
Labels:
cap came off,
dental crown
Location:
Bellevue, WA, USA
Tuesday, January 5, 2016
why do my gums bleed?
 |
| Bleeding Gums |
Why do my gums bleed? Common complaint patients say to me is their gums bleed when brushing their teeth or when they are flossing. And as such bleeding gums is often a sign of bacterial infection and gingival irritation.
What are some causes of bleeding gums?
- Gingivitis - Gums are irritated and may be swollen. This may be due to plaque and bacteria buildup along the gum line, and is typically from insufficient brushing and flossing.
- Periodontitis - Gums and supporting bony structures of the teeth have bacterial and calculus (hardened bacteria and plaque buildup) irritation.
- Pregnancy - Swollen and bleeding gums may occur during pregnancy due to increased level of progesterone.
- Immunosuppressants - Patients who have undergone organ transplants may be placed on medications such as cyclosporine. Cyclosporine is an immunosuppressant used in organ transplant recipients and for psoriasis. Calcium channel blocker agents such nifedipine and amlodipine have also been associated with gingival overgrowth. Nifedipine and Cyclosporine may cause drug-induced gingival overgrowth, and thus in combination with plaque buildup, this leads to bleeding gums.
How to treat bleeding gums?
Primary method would be to ensure daily habit of brushing and flossing. Regular 6month checkups and dental cleanings are helpful Main benefit of using dental floss is that it physically removes bacteria and plaque trapped in between the teeth and along the gum line. A water pick may also be a useful adjunct tool.Bleeding gums due to periodontitis may require a "deep cleaning" or root scaling and planing to remove hardened bacteria and calculus beneath the gum line. After the deep cleaning is done, more frequent maintenance cleanings and diligent at-home care may be required to prevent the calculus buildup from reoccurring.
Pregnancy induced gingival overgrowth and bleeding gums would require the patient to be extra diligent with daily brushing and flossing. After delivery when progesterone levels go back to normal levels, the gum inflammation and swelling would typically improve on its own.
For those on immunosuppressants such as cyclosporine and nifedipine, regular dental cleanings and at home daily brushing and flossing is critical to ensure optimal gum health. Good oral hygiene is critical to ensure teeth and gums stay healthy during treatment.
If you have any questions regarding why your gums bleed, be sure to consult your family dentist and hygienist.
From your gentle family dentist in Redmond and Bellevue,
Peter Chien, DMD, MPH
www.bellevuefamilydentistry.com
(425) 614-1600
Labels:
bleeding gums,
flossing,
oral hygiene,
pregnancy
Location:
Bellevue, WA, USA
Subscribe to:
Posts (Atom)